Infect
An EU-funded project ongoing between 2013-2018, supported by the FP7 Health framework.

INFECT-project, 2013-2018
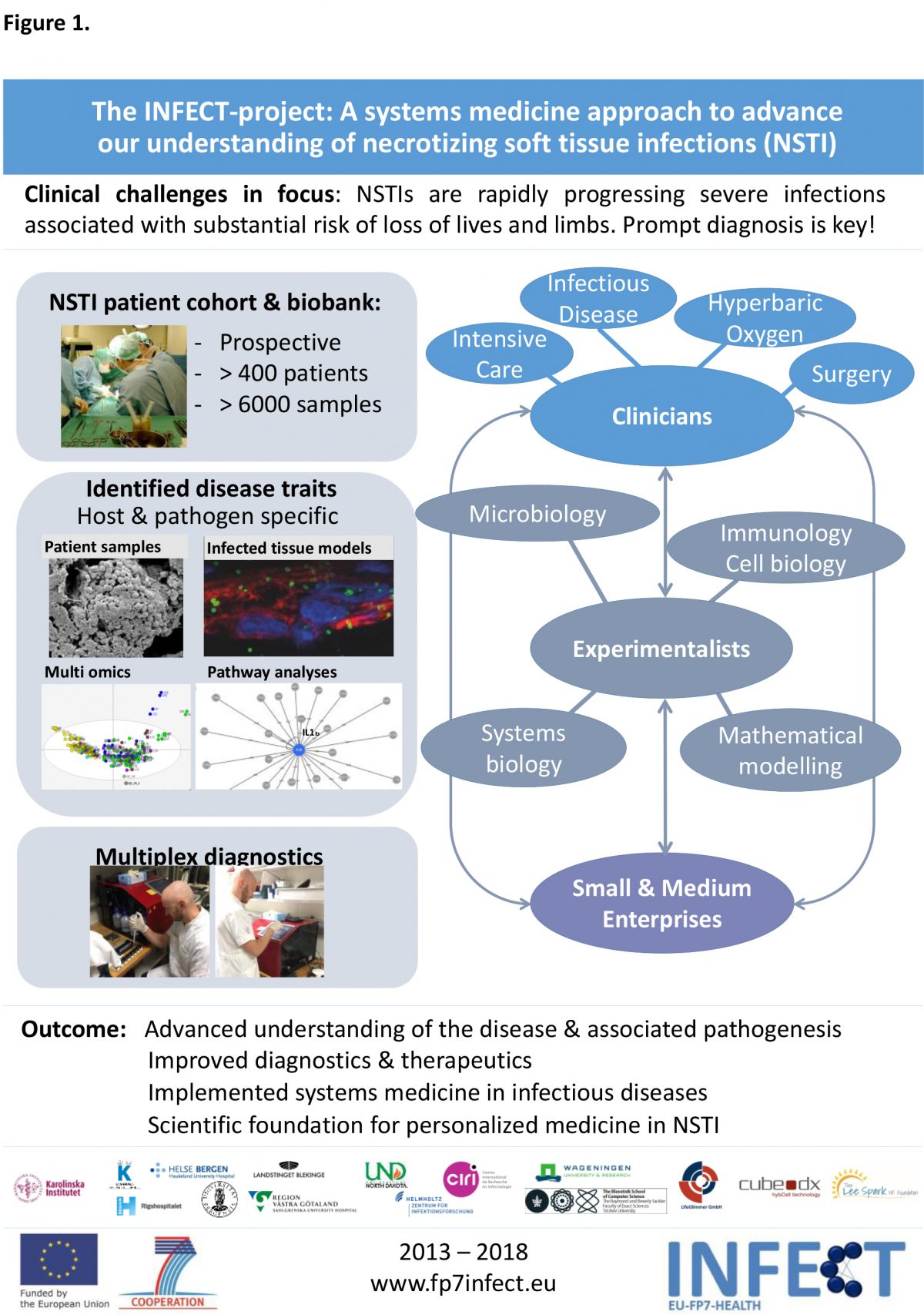
The INFECT-project included 14 multidisciplinary partners from across Europe, Israel and the US. The overall goal of the project was to advance our understanding of the pathophysiological mechanisms, prognosis, and diagnosis of the multifactorial highly lethal necrotizing soft tissue infections (NSTIs). NSTI’s are rapidly spreading infections that may cause extensive loss of soft tissue or limbs, multiorgan failure and are associated with a considerable fatality rate. There is an urgent need for novel diagnostic and therapeutic strategies in order to improve outcome of NSTIs. To achieve this, a comprehensive and integrated knowledge of diagnostic features, causative microbial agent, treatment strategies, and pathogenic mechanisms (host and bacterial disease traits and their underlying interaction network) was sought. INFECT obtained such insights through an integrated systems biology approach in patients and different clinically relevant experimental models.
Key achievements of INFECT include:
- Establishment of the world’s largest NSTI patient cohort with extended clinical registry and associated biobank providing a unique resource for the proposed studies.
- Advanced insight into the clinical aspects of NSTIs providing the basis for evidence-based guidelines for patient management and care.
- The systems medicine analyses within INFECT have substantially advanced our understanding of these life-threatening infections, including the identification of novel pathogenic mechanisms and specific host and bacterial disease traits associated with disease outcome.
- The results demonstrate that the pathophysiology of NSTI are influenced both by the causative microbe and by host factors, underscoring the need for patient stratification and implementation of tailored therapy/personalized medicine in these infections.
- Multiplex diagnostic tools for rapid pathogen identification and monitoring of disease associated biomarkers have been developed and tested in the clinical setting.
- The novel understanding of the disease mechanisms of these infections has resulted in changed clinical practice related to antibiotic usage as well as use of immunomodulatory treatments.
- Fostering the new generation of clinical and preclinical scientists within the field of systems medicine in infectious diseases.